Wednesday, March 18, 2020
Palliative Care Colleagues,
At MGH, we have been learning a great deal about the delivery of effective telehealth in the palliative care setting through our multi-center PCORI REACH PC trial of standard in person palliative care vs telehealth palliative care. We are happy to share with you some of what we have learned in case it may be useful to you and your teams who may be asked to conduct virtual visits in the context of mitigation related to COVID-19. We have found that telehealth can lend itself well to the important work that we do. Below you will find some of the resources we have used to train and support clinicians in this study. Feel free to use them in anyway that would be helpful to you.
REACH PC April Newsletter
Telehealth Visit Outline
Vicki Jackson, Jennifer Temel, Joe Greer and the rest of the REACH PC team
Wednesday, March 18, 2020 by Pallimed Editor ·
by Christian Sinclair
Update 3/19 1300 CT - Here is the link to sign onto the Slack platform for the Pallimed Un-meeting. It is open to all, so please remember it is a semi-private (aka semi-public place.) Yes you can share with other hospice and palliative care colleagues. The official hours are 5p to MN ET, but people may be in there before or after, so feel free to chat with them. Zoom video chat, and games will be later in the evening. Schedule forthcoming.
Old post below
Well, I know we all wish we were in San Diego learning from each other, seeing old friends, and making new ones, but the fact is we are not doing that. I still want to honor the spirit of the annual Pallimed Party, even though throwing a party does not feel like the right optics. So let's call it an un-meeting.
So how will this work? I'm not quite sure, so bear with me. It is going to be kind of experimental so if being an early adopter is your thing, I totally get it if you are out. But a small group of us are going to try to do something virtually. It will primarily consist of the online platform Slack and Zoom, with a couple of other add-ons. So how do you sign up? Well we are still working that out, but I wanted to get this out to the people on the email list today. So bookmark this page and keep an eye on our accounts on Twitter and Facebook for more info.
And check out #hpm chat tonight on Twitter at 8pm CT if you need some bonding with colleagues right now!
Update 3/19 1300 CT - Here is the link to sign onto the Slack platform for the Pallimed Un-meeting. It is open to all, so please remember it is a semi-private (aka semi-public place.) Yes you can share with other hospice and palliative care colleagues. The official hours are 5p to MN ET, but people may be in there before or after, so feel free to chat with them. Zoom video chat, and games will be later in the evening. Schedule forthcoming.
Old post below
Well, I know we all wish we were in San Diego learning from each other, seeing old friends, and making new ones, but the fact is we are not doing that. I still want to honor the spirit of the annual Pallimed Party, even though throwing a party does not feel like the right optics. So let's call it an un-meeting.
So how will this work? I'm not quite sure, so bear with me. It is going to be kind of experimental so if being an early adopter is your thing, I totally get it if you are out. But a small group of us are going to try to do something virtually. It will primarily consist of the online platform Slack and Zoom, with a couple of other add-ons. So how do you sign up? Well we are still working that out, but I wanted to get this out to the people on the email list today. So bookmark this page and keep an eye on our accounts on Twitter and Facebook for more info.
And check out #hpm chat tonight on Twitter at 8pm CT if you need some bonding with colleagues right now!
by Christian Sinclair ·
Tuesday, March 17, 2020
by Suzana Makowski (@suzanakm)
The guidelines outlined in the recent letter co-sponsored by Pallimed and Geripal serve as important reminders of key messages for clinicians: social distancing, handwashing, use of personal protective equipment to help flatten the curve of viral spread, adhering to protocols about screening, testing and even triaging.
I would advocate for another layer of engagement in this effort. Palliative care as a specialty is uniquely positioned to address the people who are likely to be disproportionately affected by the disease: the chronically ill and the aged. After all, this population is the demographic adult palliative care clinicians see frequently.
There is a likely double risk to this population – first from the virus itself. While the overall mortality rate of COVID19 is likely to hover around 1-2%, the mortality rate for people over 80 has been reported to be 14.8-21.9%, for patients with cardiovascular disease 10-13.2%, diabetes 7-9.2%, pulmonary disease 6.3-8%. The second risk is from the triaging that will occur if indeed the burden to the US health system is even half of what is predicted.
In this second scenario, hospitals, ICUs, will be overflowing with cases, as reported currently in Italy. The number of hospital beds per capita in the US is far less than those in many other countries. In Italy, ventilators are considered to be gold. Triaging is occurring, with an aim to prioritize intensive care, ventilator utilization for patients most likely to survive the infection, rather than those who have the greatest likelihood of a poor outcome. News articles are telling stories about older people and those with chronic conditions, being sent home. The implication is they are left alone, without resources.
As Dr. Kathy Kirkland, Chief of Palliative Care at Dartmouth Hitchcock Medical Center notes, “decision support both for individuals and also for the organization if they are in the position of deciding how to allocate scarce resources is critical in times like these, and making good decisions in the face of uncertainty is one of our areas of expertise.” There are people who will choose not to be intubated, and they likely need to know , what might they can expect. ‘No care’ should not be their perception as the ‘other option’. As palliative care experts, it is incumbent on us to define what the alternative will be.
Social distancing means providing alternatives to testing in hospitals and getting supportive care in hospitals. Visiting nursing agencies around the country are training nurses to test patients in their homes. Supporting these agencies, as well as engaging hospices to help optimize symptom management at home is crucial.
Aligned with all of this, ensuring patient’s care wishes are known and documented is perhaps more critical than ever. A fear I have heard is the perception that discussing code status will equate with no treatment or triaging out of care. I understand this fear. I remember recoiling with horror upon reading the New York Times Magazine, and then hearing the keynote at AAHPM annual assembly outline the horrific and difficult decisions made at Memorial Hospital post Katrina. Patients with DNR orders left aside or euthanized. Thankfully now POLST orders allow for distinction between code status from intensity of treatment preferences. And comfort should always be provided.
Our voice about how to help make these decisions, along with ethicists (many of us are both) can change the dialogue of triaging this pandemic. We can honor a patient’s wish to be DNR with intubation by asking of their wish, and in doing to perhaps help alleviate some of the anticipated strain on access to ventilators and non-invasive ventilator support, while actually also ensuring the patient still receives care and treatment.
Palliative care, often in partnership with the work of home health agencies and hospices is leading the innovation in telehealth to enhance care at home. Already, in the early weeks of March there has been an upswing in use of telehealth among palliative care clinicians. Patients are asking for alternatives to clinic and hospital visits – wisely, and our field is responding.
We learned at CAPC in the fall of 2019 about colleagues using encrypted conference lines to facilitate the visits, even if formal telemedicine programs are not available to a group or institution. Honestly, we have for years held family meetings where family members who are out of state or out of country join the meeting via cell phone, FaceTime, WhatsApp, Skype, or another similar program. Now the process is going to be more formal. What patient encounters can we do in this manner, compared in in the patient’s room? In some ways I can engage in a more personal way using video conferencing where my face, my expressions, my non-verbal cues can be seen rather than my body hidden from within the confines of an N95 mask and goggles, or powered air purifying respirator (PAPR).
Patient education and caregiver support is another area of our expertise. But now we need to educate and support more people. Our specialty has also been a leader in use of social media for collaboration and education of peers. How can we build on this movement and provide a platform to share best practices with lay caregivers, as well as the aides and nurses in long term care facilities who have not learned the tricks of our trade?
You know all this – but what do we do differently?
For all the strengths of our specialty, there is one area we are generally no too familiar with: the step to be proactive. We tend to be the specialty to respond when all else fails. But now, we have to step in early.
To flatten the curve of this disease, we have to use all these tools and skills in the following strategic way by partnering with our organizations, regional, and state task forces to:
1. Define processes and interventions to keep people home who would prefer to avoid hospitalization.
- POLST allows patients to choose to receive full interventions, or some, or comfort. It is not about absence of care. How can we help patients make their wishes known now, without fearing being triaged away from care they would want?
- We must support VNA and hospice agencies in their efforts to screen, test, and treat patients at home. Partnering with them in expanding telehealth visits, patient and staff education about symptom management, and other creative initiatives should be considered.
2.Being a strong voice, along with ethics, in defining and clarifying the processes of triaging patients when resource allocation is slim.
- At the bedside (or via telehealth) – we are well suited to facilitate these discussions, and support families through the tough choices, especially if a true choice is available.
- In the boardroom – we cannot allow the alternative to ICU to be ‘no care.’ If a patient with a chronic illness is dying of COVID19 complications, we know how to alleviate their breathlessness, nausea, fear, abdominal pain better than just about anyone. Those protocols need to be at the table.
- Perhaps the triage can happen before the hospital, in the community, with optimal care there. We need to be the interdisciplinary voice to facilitate the possibility of this partnership and coordination of care. We do it every day in discharge planning. Now it is time for us to bring it to the intra-organizational level.
3. Use our foundational principles.
- We have multiple frameworks for dealing with crises – Maslow’s hierarchy of needs, biopsychosocial approach, 8-domains from EPIC, etc., and a recognition of as well as embedded process of interdisciplinary collaboration like few other groups in healthcare to address not only the medical and physical needs of patients and families, but the full catastrophe of this pandemic.
- We have the voice and practiced reflect to collaborate with people who see challenges from differing points of view presenting a variety of solutions.
- We can help our health system understand how to collaborate with the wisdom embedded in our communities – not only the doctors, nurses, social workers, and chaplains we often work but even beyond. It is time to expand our interdisciplinary team. How wide? It’s your decision, based on your community.
We are called to step up, not merely to participate in the rules and recommendations recommended by the epidemiologists, infectious disease experts, and others but to come to the table with ideas and perspective to mitigate the extent of the possible challenges and alleviate the suffering our communities are about to experience.
Lastly, I do wish to address another concern. Like just about every physician and nurse, healthcare professional, we are called to step in when times get hard. There is a temptation to be a hero or even martyr of some sort. We like to be close to our patients, to hold their hands, to share a hug when needed. But now is not that time. We have to find other ways of leaning in, lending strength, being present with, other than physical closeness. For many of us, this will be hard and even feel as though we are failing our patients, or part of our own sense of purpose. The greater good must prevail right now. Remember music can touch a heart from a distance. Your skill in listening and being present can also transcend distance.
Suzana K. Everett Makowski, MD MMM CPE FAAHPM FACP comes back after a long hiatus to contribute to Pallimed again. She currently is Chief of Palliative Care at Exeter Health Resources, a community health system in New Hampshire. Having grown up internationally as a citizen of Brazil and the US, she has a passion for inter-cultural communication and collaboration in palliative care. Other areas of interest include complexity science and positive deviance, lean and culture change, leadership and innovation.
She can be found on Twitter @suzanakm
For more posts on COVID-19, click here.
For more posts on Emergency Preparedness, click here.
For more posts by Suzana Makowski, click here.
Check out the Pallimed COVID-19 Resource page here.
The guidelines outlined in the recent letter co-sponsored by Pallimed and Geripal serve as important reminders of key messages for clinicians: social distancing, handwashing, use of personal protective equipment to help flatten the curve of viral spread, adhering to protocols about screening, testing and even triaging.
I would advocate for another layer of engagement in this effort. Palliative care as a specialty is uniquely positioned to address the people who are likely to be disproportionately affected by the disease: the chronically ill and the aged. After all, this population is the demographic adult palliative care clinicians see frequently.
There is a likely double risk to this population – first from the virus itself. While the overall mortality rate of COVID19 is likely to hover around 1-2%, the mortality rate for people over 80 has been reported to be 14.8-21.9%, for patients with cardiovascular disease 10-13.2%, diabetes 7-9.2%, pulmonary disease 6.3-8%. The second risk is from the triaging that will occur if indeed the burden to the US health system is even half of what is predicted.
In this second scenario, hospitals, ICUs, will be overflowing with cases, as reported currently in Italy. The number of hospital beds per capita in the US is far less than those in many other countries. In Italy, ventilators are considered to be gold. Triaging is occurring, with an aim to prioritize intensive care, ventilator utilization for patients most likely to survive the infection, rather than those who have the greatest likelihood of a poor outcome. News articles are telling stories about older people and those with chronic conditions, being sent home. The implication is they are left alone, without resources.
As Dr. Kathy Kirkland, Chief of Palliative Care at Dartmouth Hitchcock Medical Center notes, “decision support both for individuals and also for the organization if they are in the position of deciding how to allocate scarce resources is critical in times like these, and making good decisions in the face of uncertainty is one of our areas of expertise.” There are people who will choose not to be intubated, and they likely need to know , what might they can expect. ‘No care’ should not be their perception as the ‘other option’. As palliative care experts, it is incumbent on us to define what the alternative will be.
Social distancing means providing alternatives to testing in hospitals and getting supportive care in hospitals. Visiting nursing agencies around the country are training nurses to test patients in their homes. Supporting these agencies, as well as engaging hospices to help optimize symptom management at home is crucial.
Aligned with all of this, ensuring patient’s care wishes are known and documented is perhaps more critical than ever. A fear I have heard is the perception that discussing code status will equate with no treatment or triaging out of care. I understand this fear. I remember recoiling with horror upon reading the New York Times Magazine, and then hearing the keynote at AAHPM annual assembly outline the horrific and difficult decisions made at Memorial Hospital post Katrina. Patients with DNR orders left aside or euthanized. Thankfully now POLST orders allow for distinction between code status from intensity of treatment preferences. And comfort should always be provided.
Our voice about how to help make these decisions, along with ethicists (many of us are both) can change the dialogue of triaging this pandemic. We can honor a patient’s wish to be DNR with intubation by asking of their wish, and in doing to perhaps help alleviate some of the anticipated strain on access to ventilators and non-invasive ventilator support, while actually also ensuring the patient still receives care and treatment.
Palliative care, often in partnership with the work of home health agencies and hospices is leading the innovation in telehealth to enhance care at home. Already, in the early weeks of March there has been an upswing in use of telehealth among palliative care clinicians. Patients are asking for alternatives to clinic and hospital visits – wisely, and our field is responding.
We learned at CAPC in the fall of 2019 about colleagues using encrypted conference lines to facilitate the visits, even if formal telemedicine programs are not available to a group or institution. Honestly, we have for years held family meetings where family members who are out of state or out of country join the meeting via cell phone, FaceTime, WhatsApp, Skype, or another similar program. Now the process is going to be more formal. What patient encounters can we do in this manner, compared in in the patient’s room? In some ways I can engage in a more personal way using video conferencing where my face, my expressions, my non-verbal cues can be seen rather than my body hidden from within the confines of an N95 mask and goggles, or powered air purifying respirator (PAPR).
Patient education and caregiver support is another area of our expertise. But now we need to educate and support more people. Our specialty has also been a leader in use of social media for collaboration and education of peers. How can we build on this movement and provide a platform to share best practices with lay caregivers, as well as the aides and nurses in long term care facilities who have not learned the tricks of our trade?
You know all this – but what do we do differently?
For all the strengths of our specialty, there is one area we are generally no too familiar with: the step to be proactive. We tend to be the specialty to respond when all else fails. But now, we have to step in early.
To flatten the curve of this disease, we have to use all these tools and skills in the following strategic way by partnering with our organizations, regional, and state task forces to:
1. Define processes and interventions to keep people home who would prefer to avoid hospitalization.
- POLST allows patients to choose to receive full interventions, or some, or comfort. It is not about absence of care. How can we help patients make their wishes known now, without fearing being triaged away from care they would want?
- We must support VNA and hospice agencies in their efforts to screen, test, and treat patients at home. Partnering with them in expanding telehealth visits, patient and staff education about symptom management, and other creative initiatives should be considered.
2.Being a strong voice, along with ethics, in defining and clarifying the processes of triaging patients when resource allocation is slim.
- At the bedside (or via telehealth) – we are well suited to facilitate these discussions, and support families through the tough choices, especially if a true choice is available.
- In the boardroom – we cannot allow the alternative to ICU to be ‘no care.’ If a patient with a chronic illness is dying of COVID19 complications, we know how to alleviate their breathlessness, nausea, fear, abdominal pain better than just about anyone. Those protocols need to be at the table.
- Perhaps the triage can happen before the hospital, in the community, with optimal care there. We need to be the interdisciplinary voice to facilitate the possibility of this partnership and coordination of care. We do it every day in discharge planning. Now it is time for us to bring it to the intra-organizational level.
3. Use our foundational principles.
- We have multiple frameworks for dealing with crises – Maslow’s hierarchy of needs, biopsychosocial approach, 8-domains from EPIC, etc., and a recognition of as well as embedded process of interdisciplinary collaboration like few other groups in healthcare to address not only the medical and physical needs of patients and families, but the full catastrophe of this pandemic.
- We have the voice and practiced reflect to collaborate with people who see challenges from differing points of view presenting a variety of solutions.
- We can help our health system understand how to collaborate with the wisdom embedded in our communities – not only the doctors, nurses, social workers, and chaplains we often work but even beyond. It is time to expand our interdisciplinary team. How wide? It’s your decision, based on your community.
We are called to step up, not merely to participate in the rules and recommendations recommended by the epidemiologists, infectious disease experts, and others but to come to the table with ideas and perspective to mitigate the extent of the possible challenges and alleviate the suffering our communities are about to experience.
Lastly, I do wish to address another concern. Like just about every physician and nurse, healthcare professional, we are called to step in when times get hard. There is a temptation to be a hero or even martyr of some sort. We like to be close to our patients, to hold their hands, to share a hug when needed. But now is not that time. We have to find other ways of leaning in, lending strength, being present with, other than physical closeness. For many of us, this will be hard and even feel as though we are failing our patients, or part of our own sense of purpose. The greater good must prevail right now. Remember music can touch a heart from a distance. Your skill in listening and being present can also transcend distance.
Suzana K. Everett Makowski, MD MMM CPE FAAHPM FACP comes back after a long hiatus to contribute to Pallimed again. She currently is Chief of Palliative Care at Exeter Health Resources, a community health system in New Hampshire. Having grown up internationally as a citizen of Brazil and the US, she has a passion for inter-cultural communication and collaboration in palliative care. Other areas of interest include complexity science and positive deviance, lean and culture change, leadership and innovation.
She can be found on Twitter @suzanakm
For more posts on COVID-19, click here.
For more posts on Emergency Preparedness, click here.
For more posts by Suzana Makowski, click here.
Check out the Pallimed COVID-19 Resource page here.
Tuesday, March 17, 2020 by Pallimed Editor ·
By Lyle Fettig @fettiglyle
Check out the Pallimed COVID-19 Resource page here. - Ed.
I love the letter co-published by Pallimed and Geripal about COVID,and you should read that too. As an erstwhile (for now) Pallimed contributor, I thought I'd toss in my two cents with some additional thoughts/reflections based on week 1 of preparing for the COVID pandemic as a palliative care physician.
Over the last week, I've operated mentally in most of these lanes:
1. Primary prevention and public health: Through extensive advocacy for social distancing and widespread testing. I have talked about it with my patients and my own family and friends. This also included persistently calling governmental officials, pulling my sons out of school, writing letters, and re-entering social media after an over two year hiatus
2. Assessment of patients with suspected COVID-19, like a person I've been following for 4-5 years who had pneumonia last year and called with complaint of a cough. The usual clinical reasoning of the scenario was complicated as I tried to balance the desire to get him evaluated with the public health considerations.
3. Management of mildly ill confirmed cases and mitigating the public health risk. Haven't dealt with this yet. Just waiting for the first call on one of my high risk clinic patients to have this. I know that even if they have mild symptoms, they might progress to lane 4. It feels unfair to think that an emerging infectious disease would take any of their lives.
4. Management of seriously or critically ill patients who might die. We've spent a lot of time with our critical care colleagues over the last week, swiftly trying to figure out what we would do with a "surge" and how it would change our usual collaboration, which is robust and well established. Enter the age of inpatient teleconsults, including a first: A surrogate asking me if he could email me a photo of himself so I could see what he looks like.
5. Worst case scenario of resource allocation issues: We hate talking about this, but it might happen, and we have to face it and be prepared.
It's dizzying to think about all of these lanes, on top of the usual issues our patients and teams face. Lane 4 and 5 are scary enough to serve as motivation to put a lot of attention into lane 1. Even though our ICU is a place with plenty of windows and sunlight, for some reason, I imagine lane 4 and 5 as a dark windowless place without walls, just a massive ward full of despair. It's enough to move any of us to tears and action.
I've found it helpful, in conversation about the pandemic, to identify which lane we are talking about at that moment, especially with respect to lane 4 vs. 5. In lane 5, there will be factors out of our control that determine whether patients get what they need. Routine palliative care practice (fueled by extra coffee and fewer administrative meetings) will serve our patients and their families well. Under any circumstance, we will do what we can to support shared decision-making, even if there are factors out of our control (as there always are).
Here are a few thoughts as we enter the new week:
Let's keep advocating in lane 1 while we prepare
It's surreal to see cars on the road and just feel, well, disturbed. After I finished pumping gas today, I wiped the handle off with Chlorox and went onto the next pump to wipe that one down too. (What have I become?) We are still woefully under testing for SARS-CoV2. Still some people think this is a nothingburger. Continue to educate patiently and figure out what's hardest for them about social distancing, and empathize. I'm struggling with it. I've been avoiding touching my family, changing clothes in the garage before entering, etc. It's for the birds.
Remember the concept of mortality salience and terror management theory
I'm scared. For myself, for my own health. It's tempered by probabilities, but you know, anecdotes. I'm scared for my family's health, and my parents are hunkered down, not even allowed to touch their mail. For the health and comfort of my current patients and their families. For the suffering that our new patients in this time period of isolation. Loneliness is already an epidemic, and the pandemic will amplify this. "Comfort and company" is essential to the end of life experience, as one of my mentors Greg Sachs likes to say. The thought of having a large number of people dying in uber-isolation, swimming in PPE, without their families.
I know I'm not alone. I've talked to colleagues about the three levels of fear: for our patients, personal, and professional. Everyone is walking around with extra fear.
What does evidence for Terror Management Theory suggest about what this will do to us? When people are confronted with their mortality, there's evidence to suggest they act in heightened ways consistent with their own values. (There was the famous study where judges handed out worse punishments for criminals after being reminded of their own mortality) It may make us more protective of those values as well. In stressful times, there's more likely to be tension about little things. Pause and make sure you're not actually on the same page about the values. In times like this, there may be uncertainty about the best means to accomplish certain goals. It helps to solidify agreement about the goal or value itself. "What we both value is..." This is the VitalTalk "align" statement from REMAP. It works for us as well as our patients and families.
Don't let perfection be the enemy of the good
Remember the secret sauce of palliative care
 What's the secret sauce? There is more than one ingredient, but in addition to all the skilled professionals from various disciplines who bring compassion and persistence to care of individuals, I think the sauce is Relational Coordination. Timely, accurate, frequent, and problem solving communication that is oriented around shared goals, shared knowledge, and mutual respect. Lean on these in the days and weeks ahead: With teammates, colleagues, hospital leaders, and most of all, patients and families.
What's the secret sauce? There is more than one ingredient, but in addition to all the skilled professionals from various disciplines who bring compassion and persistence to care of individuals, I think the sauce is Relational Coordination. Timely, accurate, frequent, and problem solving communication that is oriented around shared goals, shared knowledge, and mutual respect. Lean on these in the days and weeks ahead: With teammates, colleagues, hospital leaders, and most of all, patients and families.
Relational coordination defines the collaboration between palliative care and critical care at many places, and I can't imagine my career without this collaboration. I have a deep admiration for the critical care physicians I work with, many who have become friends over the years, sharing in the care of some of our sickest and most vulnerable patients and their families. Much has been written about avoiding war metaphors (with cancer and such), but I'm setting aside my pacifist ways for this virus. We're going to war now, locked arm and arm against this tiny alien and the cascading effect on individuals and society. The relationships built between colleagues will help us find our way through.
Let's save as many lives as we can and palliate this broken world along the way.
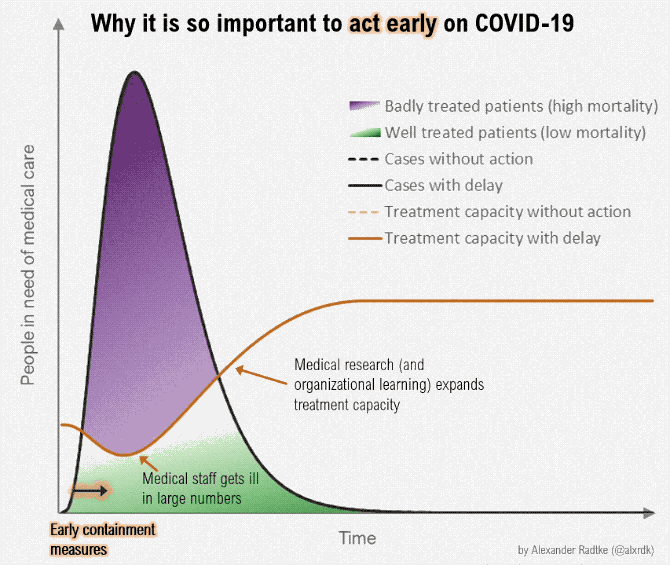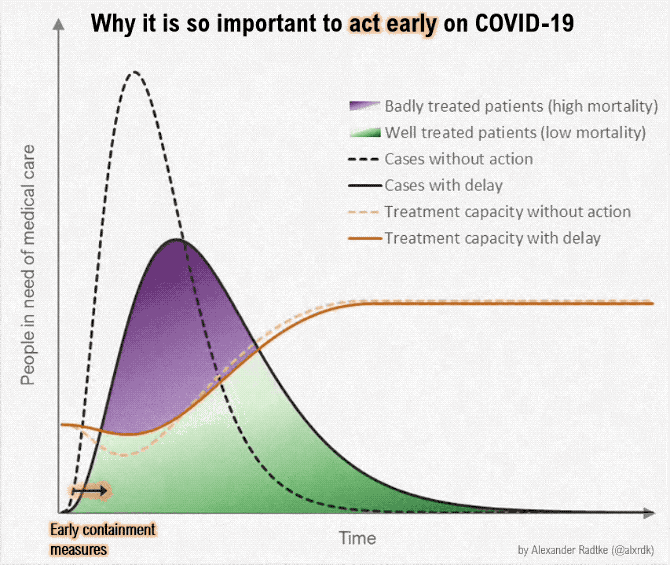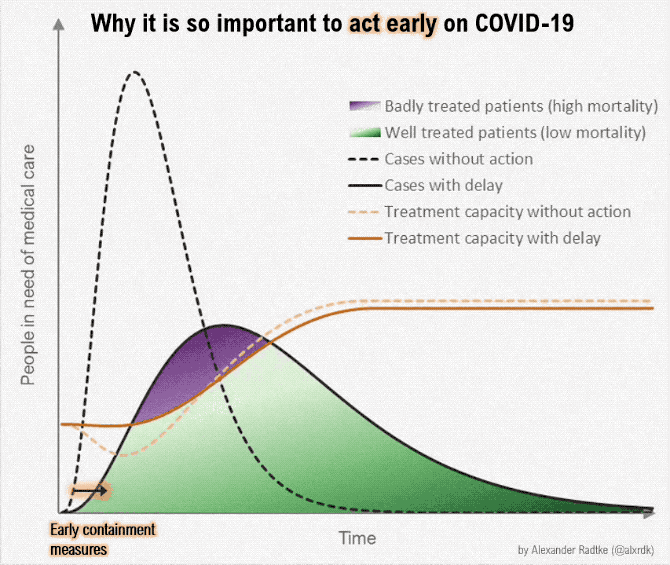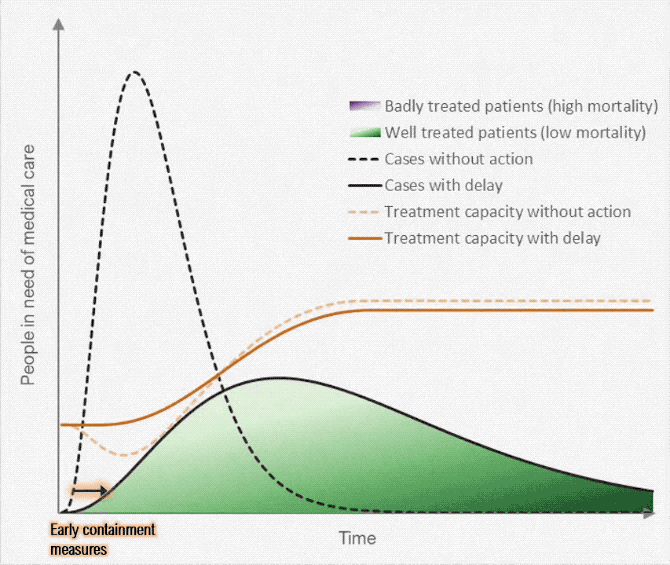
Flatten the curve, but when it hits, charge up the hill.
Source for image 1: Meredith MacMartin
Source for image 2: https://heller.brandeis.edu/relational-coordination/
Dr. Lyle Fettig is an Assistant Professor of Clinical Medicine in the Department of Medicine/Division of General Internal Medicine and Geriatrics. Dr. Fettig directs the IUSM Palliative Medicine Fellowship and works clinically with the Eskenazi Health Palliative Care Program.
For more posts on COVID-19, click here.
For more posts on Emergency Preparedness, click here.
For more posts by Lyle Fettig, click here.
Check out the Pallimed COVID-19 Resource page here. - Ed.
I love the letter co-published by Pallimed and Geripal about COVID,and you should read that too. As an erstwhile (for now) Pallimed contributor, I thought I'd toss in my two cents with some additional thoughts/reflections based on week 1 of preparing for the COVID pandemic as a palliative care physician.
Over the last week, I've operated mentally in most of these lanes:
1. Primary prevention and public health: Through extensive advocacy for social distancing and widespread testing. I have talked about it with my patients and my own family and friends. This also included persistently calling governmental officials, pulling my sons out of school, writing letters, and re-entering social media after an over two year hiatus
2. Assessment of patients with suspected COVID-19, like a person I've been following for 4-5 years who had pneumonia last year and called with complaint of a cough. The usual clinical reasoning of the scenario was complicated as I tried to balance the desire to get him evaluated with the public health considerations.
3. Management of mildly ill confirmed cases and mitigating the public health risk. Haven't dealt with this yet. Just waiting for the first call on one of my high risk clinic patients to have this. I know that even if they have mild symptoms, they might progress to lane 4. It feels unfair to think that an emerging infectious disease would take any of their lives.
4. Management of seriously or critically ill patients who might die. We've spent a lot of time with our critical care colleagues over the last week, swiftly trying to figure out what we would do with a "surge" and how it would change our usual collaboration, which is robust and well established. Enter the age of inpatient teleconsults, including a first: A surrogate asking me if he could email me a photo of himself so I could see what he looks like.
5. Worst case scenario of resource allocation issues: We hate talking about this, but it might happen, and we have to face it and be prepared.
It's dizzying to think about all of these lanes, on top of the usual issues our patients and teams face. Lane 4 and 5 are scary enough to serve as motivation to put a lot of attention into lane 1. Even though our ICU is a place with plenty of windows and sunlight, for some reason, I imagine lane 4 and 5 as a dark windowless place without walls, just a massive ward full of despair. It's enough to move any of us to tears and action.
I've found it helpful, in conversation about the pandemic, to identify which lane we are talking about at that moment, especially with respect to lane 4 vs. 5. In lane 5, there will be factors out of our control that determine whether patients get what they need. Routine palliative care practice (fueled by extra coffee and fewer administrative meetings) will serve our patients and their families well. Under any circumstance, we will do what we can to support shared decision-making, even if there are factors out of our control (as there always are).
Here are a few thoughts as we enter the new week:
Let's keep advocating in lane 1 while we prepare
It's surreal to see cars on the road and just feel, well, disturbed. After I finished pumping gas today, I wiped the handle off with Chlorox and went onto the next pump to wipe that one down too. (What have I become?) We are still woefully under testing for SARS-CoV2. Still some people think this is a nothingburger. Continue to educate patiently and figure out what's hardest for them about social distancing, and empathize. I'm struggling with it. I've been avoiding touching my family, changing clothes in the garage before entering, etc. It's for the birds.
Remember the concept of mortality salience and terror management theory
I'm scared. For myself, for my own health. It's tempered by probabilities, but you know, anecdotes. I'm scared for my family's health, and my parents are hunkered down, not even allowed to touch their mail. For the health and comfort of my current patients and their families. For the suffering that our new patients in this time period of isolation. Loneliness is already an epidemic, and the pandemic will amplify this. "Comfort and company" is essential to the end of life experience, as one of my mentors Greg Sachs likes to say. The thought of having a large number of people dying in uber-isolation, swimming in PPE, without their families.
I know I'm not alone. I've talked to colleagues about the three levels of fear: for our patients, personal, and professional. Everyone is walking around with extra fear.
What does evidence for Terror Management Theory suggest about what this will do to us? When people are confronted with their mortality, there's evidence to suggest they act in heightened ways consistent with their own values. (There was the famous study where judges handed out worse punishments for criminals after being reminded of their own mortality) It may make us more protective of those values as well. In stressful times, there's more likely to be tension about little things. Pause and make sure you're not actually on the same page about the values. In times like this, there may be uncertainty about the best means to accomplish certain goals. It helps to solidify agreement about the goal or value itself. "What we both value is..." This is the VitalTalk "align" statement from REMAP. It works for us as well as our patients and families.
Don't let perfection be the enemy of the good
"Be fast, have no regrets."— Sky News (@SkyNews) March 13, 2020
Dr Michael J Ryan says "the greatest error is not to move" and "speed trumps perfection" when it comes to dealing with an outbreak such as #coronavirus.
Get the latest on COVID-19 👉 https://t.co/HMPNwaVk37 pic.twitter.com/wDa7XOMw8Q
Remember the secret sauce of palliative care
 What's the secret sauce? There is more than one ingredient, but in addition to all the skilled professionals from various disciplines who bring compassion and persistence to care of individuals, I think the sauce is Relational Coordination. Timely, accurate, frequent, and problem solving communication that is oriented around shared goals, shared knowledge, and mutual respect. Lean on these in the days and weeks ahead: With teammates, colleagues, hospital leaders, and most of all, patients and families.
What's the secret sauce? There is more than one ingredient, but in addition to all the skilled professionals from various disciplines who bring compassion and persistence to care of individuals, I think the sauce is Relational Coordination. Timely, accurate, frequent, and problem solving communication that is oriented around shared goals, shared knowledge, and mutual respect. Lean on these in the days and weeks ahead: With teammates, colleagues, hospital leaders, and most of all, patients and families. Relational coordination defines the collaboration between palliative care and critical care at many places, and I can't imagine my career without this collaboration. I have a deep admiration for the critical care physicians I work with, many who have become friends over the years, sharing in the care of some of our sickest and most vulnerable patients and their families. Much has been written about avoiding war metaphors (with cancer and such), but I'm setting aside my pacifist ways for this virus. We're going to war now, locked arm and arm against this tiny alien and the cascading effect on individuals and society. The relationships built between colleagues will help us find our way through.
Let's save as many lives as we can and palliate this broken world along the way.
Flatten the curve, but when it hits, charge up the hill.
Source for image 1: Meredith MacMartin
Source for image 2: https://heller.brandeis.edu/relational-coordination/
Dr. Lyle Fettig is an Assistant Professor of Clinical Medicine in the Department of Medicine/Division of General Internal Medicine and Geriatrics. Dr. Fettig directs the IUSM Palliative Medicine Fellowship and works clinically with the Eskenazi Health Palliative Care Program.
For more posts on COVID-19, click here.
For more posts on Emergency Preparedness, click here.
For more posts by Lyle Fettig, click here.
by Lyle Fettig ·
Friday, March 13, 2020
Co-published March 13th on GeriPal and Pallimed
Dear Hospice and Palliative Care community,
We are sad we cannot be together this year at the Annual Assembly and deeply concerned about the growing risk of the novel coronavirus. We want to send you a bit of encouragement, and some thoughts on how we can take care of ourselves, our teams, and our community in the setting of this new pandemic.
We have always “punched above our weight” as a field, and the secret to that has been hard work, community, and being smart.
We don’t have to tell you to work hard. You and your teams know how to do this.
1) Start social distancing from others (except patients) now, wherever you are in the country. While we realize this is a stronger recommendation than currently being asked for by many public health entities, we are doing so in the interest of health care workers and patients
--COVID-19 is spreading rapidly, sometimes with minor or no symptoms, with serious impact to healthcare systems worldwide. The exponential growth in cases in China, Italy, and South Korea has overwhelmed the healthcare systems, and has affected our patient population most seriously - the chronically ill and older adults.
--We need to be ready and able to respond when the time comes. We will be exposed to the COVID–19 virus, and we cannot afford to lose our hospice and palliative care clinicians to isolation restrictions or illness, especially given the workforce shortages many of us face already.
--Stay away from public gatherings like movies, sporting events, concerts, the theater, houses of worship and other places where people assemble. Try to participate in these from home via electronic means, if possible. Talk with your spiritual leaders about making services available via streaming tech, for example.
--Attend all meetings electronically unless physical presence is absolutely necessary. Replace non–essential meetings with email or other asynchronous communications,
--Eliminate all non–essential travel, and
--Protect yourself at work using PPE and rigorous technique. *Reminder of how to safely don and doff PPE here
2) Follow all local, state and national guidelines for COVID-19. This is critical as there are regional differences. However these hold true.
--Wash your hands or use at least 60% alcohol hand sanitizer
--Avoid touching your face. (Holly finds this impossible, so she wears her hair up and bobby pinned normally, to avoid itching her face and tucking her hair behind her ear constantly.)
--Stay home if you are sick, until the symptoms are gone for at least 24 hours. (This is hard as we have been trained to just work anyway. Don’t do it. Stay home.)
--If you are exposed and/or have COVID-19 symptoms, you should isolate at home for 14 days. If you think you should be tested, make sure you call ahead and know how your region is handling testing for health care workers. (You should have received copious emails from your institutions on this. If not, contact your institution's occupational health team or COVID response team for local instructions on how to access testing.)
--If you have traveled to or had a layover in any of the 5 countries (China, Iran, Italy, South Korea, or Japan) then you need to stay in isolation at home even if you are asymptomatic. Note these countries may change after this is originally posted on Mar 12, 2020.
--See CDC for the latest guidelines: www.coronavirus.gov
--Wash your hands the right way. (Yeah, we said it already).
3) For hospices and home-based palliative care:
--NHPCO has an excellent resource page for that includes CDC guidance for hospices on COVID-19 infection control and prevention : https://www.nhpco.org/coronavirus
--Proactively provide education to your patients and their caregivers on how to stay safe and get food, medication, pet food, household goods, and other necessities, including companies that deliver to minimize household exposure. You may deliver the patient’s medications, but their caregivers will also need to get their medications.
--Proactively remind patients and caregivers about CDC guidelines (e.g. handwashing, greeting people, etc.), and to clean their cell phones.
--Consider having non-caregiver loved ones Facetime or Skype to “visit” rather than coming in person.
--Use virtual visits whenever possible.
--For patients who need to be seen, send only the necessary team members.
--Call ahead to screen for exposure and symptoms of the patient or caregivers to see if PPE is necessary.
--Ensure your team members have appropriate PPE in their cars, as well as disposal containers. Consider donning and doffing the PPE in attached garages or entryways to help maintain patient privacy.
--Make sure people going into homes know how to don/doff PPE and are FIT tested, if appropriate.
--Wash hands or use hand sanitizer prior to and after seeing patients.
--Wipe down all equipment and cell phones before and after each patient.
--Follow all guidelines for facilities and minimize in-person visits to only needed personnel.
--Don’t let fear prevent appropriate patient care.
4) For ambulatory palliative care:
--Proactively provide education to your patients and their caregivers on how to stay safe and get food, medication, pet food, household goods, and other necessities, including companies that deliver to minimize household exposure.
--Remind patients and caregivers about CDC guidelines (e.g. handwashing, greeting people, etc.) and to clean their cell phones.
--Consider having non-caregiver loved ones Facetime or Skype to “visit” rather than coming in person.
--Screen all patients and caregivers for symptoms or exposure when calling to remind them of their appointment.
--If URI or COVID symptoms, follow your institutional guidelines about home isolation and testing.
--Consider which patients’ needs can be met with virtual or telephone visits.
--Work with your institution to implement HIPAA approved telehealth visit capabilities if you do not have them. Understanding some telehealth visits cannot be reimbursed, talk with your colleagues and health system about what amount of service can be feasibly provided without guarantee of reimbursement.
--Consider which team members really need to be in the room, versus can call to provide information or support.
--For now, do not require that patients be seen at a certain frequency for controlled substance monitoring if it can be safely done for a particular patient, unless required by law or regulation.
--Don’t let fear prevent appropriate patient care.
5) For inpatient palliative care:
--Provide education to your patients’ caregivers on how to stay safe and get food, medication, pet food, household goods, and other necessities, including companies that deliver to minimize household exposure for when the patient is discharged.
--Remind patients and caregivers about CDC guidelines (e.g. handwashing, greeting people, etc.) and to clean their cell phones.
--Consider having loved ones call, Facetime, or Skype to “visit” rather than coming in person, if they even are allowed into the hospital.
--Consider having physicians, NPs, and PAs who are at home in isolation due to a cold, travel, or COVID exposure, be a triage/advice person for your consult service. Palliative care teams are often at capacity without an epidemic, so with COVID we may need to give recommendations to non-palliative clinicians (e.g. teleconsults or curbsides) when we can, and only see the patients who need our in-person services.
--Establish and update what a “patient who needs your service” means as a team at each site, so there is not confusion if the definition changes during a surge. For a palliative care team covering multiple hospitals, consider asking for emergency privileges now at all the hospitals, so all clinicians can flexibly cover hospitals they don’t normally practice in.
--Make sure your institution is planning for symptom management needs, like opioids and benzodiazepines for dyspnea and anxiety.
--Be prepared to offer virtual bereavement support to families who are not allowed to be with critically ill patients.
--Support other teams in the hospital, everyone will be stressed and a kind word or offer to help may go a long way.
--Don’t let fear prevent appropriate patient care.
6) For Program Directors:
--Consider going virtual for education and fellow support.
--Have the trainees see the non-COVID cases, to minimize their exposure and conserve PPE. Attending physicians will need to see the patients, and can teach about COVID outside the room, so the trainees don’t lose out on the learning.
--Consider extra support, like virtual video check-in’s, or more frequent texts/ or calls about the fellows’ well-being, given the stress on the system.
--Make sure your fellows can get food and necessities, and have a place to go, if they are asked to isolate
And as all us hopefully do, prioritize kindness. There are reports of xenophobia behaviors, and shunning of people with COVID, and with heightened emotions we may need to remind people we ALL do better when we care for each other and treat each other equally.
Finally... together we can do this. As hospice and palliative care people, we understand the value of team. And right now we are all on each other's team. While we may be social distancing, we have a vibrant virtual community, as well your home community. AAHPM has Connect, we can find each other at the #hapc hashtag on Twitter, or at the #hpm tweetchat. Take care of you, take care of each other.
Much love folks. Let’s be safe, and let’s be prepared.
Strong back, soft front. Deep breath. Stay grounded.
Holly Yang, Alex Smith, Christian Sinclair, Eric Widera, Paul Tatum, Drew Rosielle
For more posts on COVID-19, click here.
For more posts on Emergency Preparedness, click here.
Check out the Pallimed COVID-19 Resource page here.
Resources: NHPCO - COVID-19 Information
CMS - CMS Actionable Guidance to Providers about COVID-19 Virus
Dear Hospice and Palliative Care community,
We are sad we cannot be together this year at the Annual Assembly and deeply concerned about the growing risk of the novel coronavirus. We want to send you a bit of encouragement, and some thoughts on how we can take care of ourselves, our teams, and our community in the setting of this new pandemic.
We have always “punched above our weight” as a field, and the secret to that has been hard work, community, and being smart.
We don’t have to tell you to work hard. You and your teams know how to do this.
1) Start social distancing from others (except patients) now, wherever you are in the country. While we realize this is a stronger recommendation than currently being asked for by many public health entities, we are doing so in the interest of health care workers and patients
--COVID-19 is spreading rapidly, sometimes with minor or no symptoms, with serious impact to healthcare systems worldwide. The exponential growth in cases in China, Italy, and South Korea has overwhelmed the healthcare systems, and has affected our patient population most seriously - the chronically ill and older adults.
--We need to be ready and able to respond when the time comes. We will be exposed to the COVID–19 virus, and we cannot afford to lose our hospice and palliative care clinicians to isolation restrictions or illness, especially given the workforce shortages many of us face already.
--Stay away from public gatherings like movies, sporting events, concerts, the theater, houses of worship and other places where people assemble. Try to participate in these from home via electronic means, if possible. Talk with your spiritual leaders about making services available via streaming tech, for example.
--Attend all meetings electronically unless physical presence is absolutely necessary. Replace non–essential meetings with email or other asynchronous communications,
--Eliminate all non–essential travel, and
--Protect yourself at work using PPE and rigorous technique. *Reminder of how to safely don and doff PPE here
2) Follow all local, state and national guidelines for COVID-19. This is critical as there are regional differences. However these hold true.
--Wash your hands or use at least 60% alcohol hand sanitizer
--Avoid touching your face. (Holly finds this impossible, so she wears her hair up and bobby pinned normally, to avoid itching her face and tucking her hair behind her ear constantly.)
--Stay home if you are sick, until the symptoms are gone for at least 24 hours. (This is hard as we have been trained to just work anyway. Don’t do it. Stay home.)
--If you are exposed and/or have COVID-19 symptoms, you should isolate at home for 14 days. If you think you should be tested, make sure you call ahead and know how your region is handling testing for health care workers. (You should have received copious emails from your institutions on this. If not, contact your institution's occupational health team or COVID response team for local instructions on how to access testing.)
--If you have traveled to or had a layover in any of the 5 countries (China, Iran, Italy, South Korea, or Japan) then you need to stay in isolation at home even if you are asymptomatic. Note these countries may change after this is originally posted on Mar 12, 2020.
--See CDC for the latest guidelines: www.coronavirus.gov
--Wash your hands the right way. (Yeah, we said it already).
3) For hospices and home-based palliative care:
--NHPCO has an excellent resource page for that includes CDC guidance for hospices on COVID-19 infection control and prevention : https://www.nhpco.org/coronavirus
--Proactively provide education to your patients and their caregivers on how to stay safe and get food, medication, pet food, household goods, and other necessities, including companies that deliver to minimize household exposure. You may deliver the patient’s medications, but their caregivers will also need to get their medications.
--Proactively remind patients and caregivers about CDC guidelines (e.g. handwashing, greeting people, etc.), and to clean their cell phones.
--Consider having non-caregiver loved ones Facetime or Skype to “visit” rather than coming in person.
--Use virtual visits whenever possible.
--For patients who need to be seen, send only the necessary team members.
--Call ahead to screen for exposure and symptoms of the patient or caregivers to see if PPE is necessary.
--Ensure your team members have appropriate PPE in their cars, as well as disposal containers. Consider donning and doffing the PPE in attached garages or entryways to help maintain patient privacy.
--Make sure people going into homes know how to don/doff PPE and are FIT tested, if appropriate.
--Wash hands or use hand sanitizer prior to and after seeing patients.
--Wipe down all equipment and cell phones before and after each patient.
--Follow all guidelines for facilities and minimize in-person visits to only needed personnel.
--Don’t let fear prevent appropriate patient care.
4) For ambulatory palliative care:
--Proactively provide education to your patients and their caregivers on how to stay safe and get food, medication, pet food, household goods, and other necessities, including companies that deliver to minimize household exposure.
--Remind patients and caregivers about CDC guidelines (e.g. handwashing, greeting people, etc.) and to clean their cell phones.
--Consider having non-caregiver loved ones Facetime or Skype to “visit” rather than coming in person.
--Screen all patients and caregivers for symptoms or exposure when calling to remind them of their appointment.
--If URI or COVID symptoms, follow your institutional guidelines about home isolation and testing.
--Consider which patients’ needs can be met with virtual or telephone visits.
--Work with your institution to implement HIPAA approved telehealth visit capabilities if you do not have them. Understanding some telehealth visits cannot be reimbursed, talk with your colleagues and health system about what amount of service can be feasibly provided without guarantee of reimbursement.
--Consider which team members really need to be in the room, versus can call to provide information or support.
--For now, do not require that patients be seen at a certain frequency for controlled substance monitoring if it can be safely done for a particular patient, unless required by law or regulation.
--Don’t let fear prevent appropriate patient care.
5) For inpatient palliative care:
--Provide education to your patients’ caregivers on how to stay safe and get food, medication, pet food, household goods, and other necessities, including companies that deliver to minimize household exposure for when the patient is discharged.
--Remind patients and caregivers about CDC guidelines (e.g. handwashing, greeting people, etc.) and to clean their cell phones.
--Consider having loved ones call, Facetime, or Skype to “visit” rather than coming in person, if they even are allowed into the hospital.
--Consider having physicians, NPs, and PAs who are at home in isolation due to a cold, travel, or COVID exposure, be a triage/advice person for your consult service. Palliative care teams are often at capacity without an epidemic, so with COVID we may need to give recommendations to non-palliative clinicians (e.g. teleconsults or curbsides) when we can, and only see the patients who need our in-person services.
--Establish and update what a “patient who needs your service” means as a team at each site, so there is not confusion if the definition changes during a surge. For a palliative care team covering multiple hospitals, consider asking for emergency privileges now at all the hospitals, so all clinicians can flexibly cover hospitals they don’t normally practice in.
--Make sure your institution is planning for symptom management needs, like opioids and benzodiazepines for dyspnea and anxiety.
--Be prepared to offer virtual bereavement support to families who are not allowed to be with critically ill patients.
--Support other teams in the hospital, everyone will be stressed and a kind word or offer to help may go a long way.
--Don’t let fear prevent appropriate patient care.
6) For Program Directors:
--Consider going virtual for education and fellow support.
--Have the trainees see the non-COVID cases, to minimize their exposure and conserve PPE. Attending physicians will need to see the patients, and can teach about COVID outside the room, so the trainees don’t lose out on the learning.
--Consider extra support, like virtual video check-in’s, or more frequent texts/ or calls about the fellows’ well-being, given the stress on the system.
--Make sure your fellows can get food and necessities, and have a place to go, if they are asked to isolate
And as all us hopefully do, prioritize kindness. There are reports of xenophobia behaviors, and shunning of people with COVID, and with heightened emotions we may need to remind people we ALL do better when we care for each other and treat each other equally.
Finally... together we can do this. As hospice and palliative care people, we understand the value of team. And right now we are all on each other's team. While we may be social distancing, we have a vibrant virtual community, as well your home community. AAHPM has Connect, we can find each other at the #hapc hashtag on Twitter, or at the #hpm tweetchat. Take care of you, take care of each other.
Much love folks. Let’s be safe, and let’s be prepared.
Strong back, soft front. Deep breath. Stay grounded.
Holly Yang, Alex Smith, Christian Sinclair, Eric Widera, Paul Tatum, Drew Rosielle
For more posts on COVID-19, click here.
For more posts on Emergency Preparedness, click here.
Check out the Pallimed COVID-19 Resource page here.
Resources: NHPCO - COVID-19 Information
CMS - CMS Actionable Guidance to Providers about COVID-19 Virus
Friday, March 13, 2020 by Pallimed Editor ·
Subscribe to:
Posts (Atom)